A refresher on this difficult-to-diagnose tick-borne disease
A horse that’s underperforming, lethargic, and repeatedly yet subtly lame—it’s one of the most frustrating scenarios for an owner. At some point in your riding career, you’ve likely encountered a horse with lameness that was either nonspecific or undiagnosed. Maybe you noticed it in one limb one day and another the next.
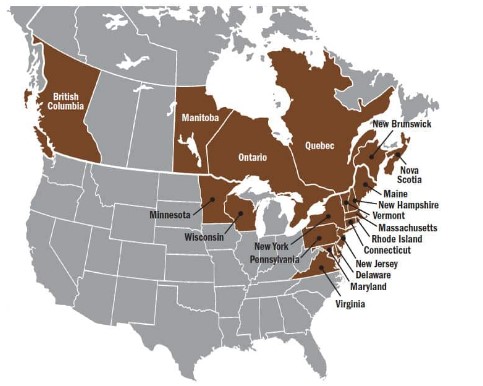
If this sounds familiar and you live in a Lyme-endemic region (see the map on the next page), someone has likely mentioned the possibility that your horse has Lyme disease. Our knowledge of equine Lyme disease, otherwise known as Borrelia burgdorferi infection, is burgeoning and nascent. Currently, there are more questions than answers in the scientific literature. So how do you and your veterinarian determine if your horse is affected? Read on to find out, based on the latest research findings and consensus statements, as well as my practical experience as a veterinary internal medicine specialist in the heart of Lyme country.
What Is It?
Lyme disease is a tick-borne infectious disease caused by the bacterium B. burgdorferi. In humans infection can lead to a wide range of clinical signs, including rashes; arthritis; skin, neurologic, and cardiac issues; and possibly prolonged fatigue. In dogs Lyme disease can also cause kidney issues. The disease is not as well-characterized in horses, however, due to the limited equine studies that exist, but researchers believe its signs include neurologic issues, uveitis (eye inflammation), cutaneous pseudolymphoma (a nodular skin disease around the tick bite), muscle atrophy (wasting), behavioral changes, hyperesthesia (excessive sensitivity to stimuli), and heart rhythm abnormalities, among others.
How Does a Horse Get It?
In North America hard-bodied (ixodid, from the family Ixodidae) ticks carry B. burgdorferi. In the East the common culprit is the deer tick or black-legged tick (Ixodes scapularis); in the West it’s the Western black-legged tick (Ixodes pacificus). These ticks have a two-year life cycle and must feed on small and large mammals’ blood to survive. Adult ticks tend to be active in the spring and fall, climbing to grass tips when temperatures rise above 40°F and attaching to animals that brush against the grass. This is typically how a tick attaches to a horse, which is a dead-end host—it cannot pass the bacteria on to humans or other animals via contact, needles, or ticks or other bloodborne vectors (intermediate hosts such as mice, squirrels, and deer, however, can serve as reservoirs for B. burgdorferi, which can be transmitted via ticks). Researchers know that after several hours of feeding, the tick will have infected that horse with B. burgdorferi. How quickly clinical signs appear, if at all, however, continues to stump them.
“Borrelia burgdorferi infection is common in horses living in Lyme-endemic areas,” says Rachel Gardner, DVM, Dipl. ACVIM, an equine internal medicine specialist at B.W. Furlong & Associates, in Oldwick, New Jersey. “However, the frequency with which horses develop clinical infection is unknown.”
According to the Centers for Disease Control and Prevention, ixodid ticks are endemic in 14 states in the Midwest and along the East Coast, as well as in six Canadian provinces. Their geographical range appears to be expanding. Because horses live primarily outdoors, they’re naturally at a higher risk of contracting Lyme disease than humans and pets. In fact, horses might be more widely exposed to the disease than we realize. Scientists at the Connecticut Agricultural Experiment Station, for instance, showed that as many as 59% of healthy horses in Connecticut and New York tested had antibodies against B. burgdorferi in their blood—indicating exposure—but did not show clinical signs of Lyme disease. Similarly, Virginia-Maryland College of Veterinary Medicine researchers found that 33% of healthy horses in Southwest Virginia tested positive for the antibodies.
Click here to see more...